The Great Retreat: How States Are Abandoning Evidence-Based Healthcare for Short-Term Budgetary Convenience
Published
- 3 min read
A Disturbing Policy Reversal
In what can only be described as a devastating policy reversal, multiple states are withdrawing Medicaid coverage for GLP-1 medications used for weight loss treatment, despite overwhelming evidence of their long-term health benefits and cost-effectiveness. This retreat comes at precisely the moment when prescriptions for these drugs have increased by an astonishing 700% between 2019 and 2023, according to data from KFF, a respected health policy research group. The numbers tell a story of both tremendous medical promise and profound policy failure: outpatient Medicaid prescriptions grew from 755,300 to 3.8 million during this period, while spending increased from $597.3 million to $3.9 billion.
The Context: Obesity as a National Health Crisis
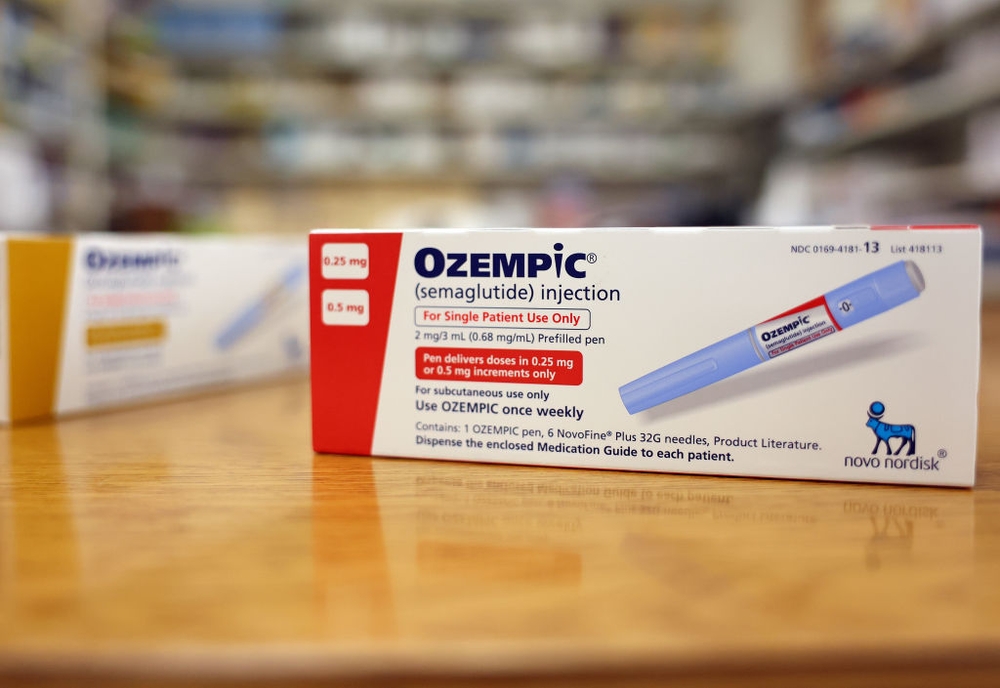
The backdrop to this policy debate is the stark reality that more than 2 in 5 American adults suffer from obesity, defined by the CDC as having a body mass index of 30 or higher. This epidemic costs the U.S. healthcare system nearly $173 billion annually and contributes significantly to chronic conditions like heart disease and diabetes. GLP-1 medications, including popular drugs like Ozempic, Wegovy, and Zepbound, have emerged as breakthrough treatments that not only help balance blood sugar levels but also curb hunger signals, enabling significant weight loss and potentially reducing obesity-related complications.
What makes this situation particularly tragic is the timing: just as these medications demonstrate unprecedented effectiveness, states are pulling back coverage. North Carolina ended Medicaid coverage for GLP-1s for obesity last month, while California, New Hampshire, and South Carolina will terminate coverage on January 1. Michigan plans to restrict coverage to only those with morbid obesity, and Pennsylvania, Rhode Island, and Wisconsin are considering similar restrictions. This represents a complete reversal from last year’s sentiment, when about half of states expressed interest in expanding coverage.
The Human Cost of Fiscal Austerity
Elizabeth Williams, a senior policy manager at KFF specializing in Medicaid, identifies the core driver of this policy shift: “recent state budget challenges and the significant, significant costs associated with coverage.” After several years of robust revenue growth following the pandemic, states now face slowing revenues and increasing spending demands, exacerbated by what Williams describes as “federal actions” creating fiscal uncertainty. The Trump administration’s decision to scrap a Biden-era proposal that would have required Medicaid programs to cover GLP-1s for obesity treatment further complicated the landscape.
But behind these budget numbers lies profound human suffering. Dr. Jennifer McCauley, a weight management physician at UNC Health, testified to the real-world consequences: “Now they’ve stopped coverage, so those people are now going back, regaining some of the weight, because they’re unable to obtain these medications, and also are suffering the health consequences of obesity.” Her words underscore the tragedy of this policy reversal—patients who had found effective treatment are being systematically abandoned.
A Fundamental Betrayal of Healthcare Principles
What we are witnessing represents nothing less than a betrayal of fundamental healthcare principles and a retreat from evidence-based medicine. The argument that these medications aren’t cost-effective because patients may regain weight if they stop treatment fundamentally misunderstands both the nature of chronic disease and the purpose of healthcare. We don’t deny insulin to diabetic patients because they’ll need it again tomorrow; we don’t withhold blood pressure medication because hypertension requires ongoing treatment. Obesity is a chronic medical condition, not a personal failing, and treating it requires sustained medical intervention.
The moral failure here is staggering. When states prioritize short-term budget concerns over long-term health outcomes, they effectively condemn vulnerable citizens to preventable suffering. James Werner, a spokesperson for North Carolina’s Department of Health and Human Services, explicitly linked the coverage change to the state legislature’s “failure to budget enough money for Medicaid.” This admission reveals the brutal calculus at work: human health has become negotiable in budget negotiations.
The Hypocrisy of Selective Healthcare Coverage
The current situation exposes a deeper hypocrisy in our healthcare system. All state Medicaid programs cover GLP-1 medications for diabetes and cardiovascular conditions—the very same drugs they’re now denying for obesity treatment. This artificial distinction between “worthy” and “unworthy” medical conditions reflects persistent stigma against obesity rather than sound medical judgment. As Dr. McCauley noted, “There are definitely vulnerable populations that probably would not be able to obtain weight loss without these medications.” By restricting access, states are effectively denying care to those who need it most.
The contrast between state actions and medical evidence couldn’t be sharper. Numerous studies, including research published in The BMJ, demonstrate both the effectiveness of these treatments and their potential for long-term healthcare savings. Yet states are retreating precisely when the evidence for comprehensive coverage is strongest. This represents a failure of both courage and vision—an unwillingness to invest in preventive care despite clear evidence of future benefits.
Alternative Approaches and Missed Opportunities
Some states are exploring more nuanced approaches that balance fiscal responsibility with patient care. Connecticut, for instance, maintains coverage for state employees but requires beneficiaries to try online weight-loss counseling first. North Dakota took a different path entirely, becoming the first state to mandate that insurers on its Affordable Care Act marketplace cover the drugs for weight loss. John Arnold, North Dakota’s Deputy Insurance Commissioner, explained the reasoning: “Our biggest concern was reducing those comorbidities and the long-term impact that that has on the cost of insurance in general.”
These alternative approaches demonstrate that creative solutions exist when policymakers prioritize both fiscal responsibility and patient health. Yet most states are choosing the path of least resistance—simply cutting coverage rather than designing smarter systems. The result is what Colleen Becker of the National Conference of State Legislatures describes as states trying to “balance access and provide that access to patients, but they’re stewards of their budgets.” This framing suggests a false choice between fiscal responsibility and patient care when innovative approaches could achieve both.
The Broader Implications for American Healthcare
This retreat from evidence-based obesity treatment reflects a broader crisis in American healthcare—our inability to think beyond short-term budget cycles and invest in preventive care. The same short-term thinking that plagues our infrastructure investment, education funding, and environmental policy now threatens to undermine healthcare outcomes for millions. When we sacrifice long-term health gains for temporary budgetary convenience, we betray not just current patients but future generations who will inherit both our fiscal decisions and their health consequences.
The human cost of these policy decisions is immeasurable. Patients who had found hope in effective treatment now face the prospect of regression and renewed health struggles. Families who had seen loved ones regain health and vitality now watch as that progress unravels. Healthcare providers like Dr. McCauley must deliver the devastating news that effective treatments are no longer available to those who need them most.
A Call for Moral Courage in Healthcare Policy
What’s needed now is not retreat but courage—the moral courage to invest in evidence-based treatments, the political courage to explain long-term benefits to constituents, and the ethical courage to prioritize human health over temporary budget concerns. The fundamental question we must answer is whether healthcare is a human right or a commodity subject to budgetary whims. Our current trajectory suggests we’re choosing the latter, and history will judge this choice harshly.
The solution requires both state and federal leadership. States must explore creative approaches like those in North Dakota and Connecticut rather than simply cutting coverage. The federal government must provide clearer guidance and support for evidence-based treatments. Most importantly, we need a public conversation that recognizes obesity as the medical condition it is, rather than a moral failing deserving of punitive treatment.
As we move forward, we must remember that healthcare policy isn’t just about numbers on a spreadsheet—it’s about human lives, human dignity, and our collective commitment to one another’s wellbeing. The current retreat from GLP-1 coverage represents a failure of that commitment, and history will record it as such. The question is whether we have the courage to change course before more lives are unnecessarily lost to preventable suffering.
