Missouri's Rural Hospital Crisis: A Dangerous Legislative Response That Puts Patients at Risk
Published
- 3 min read
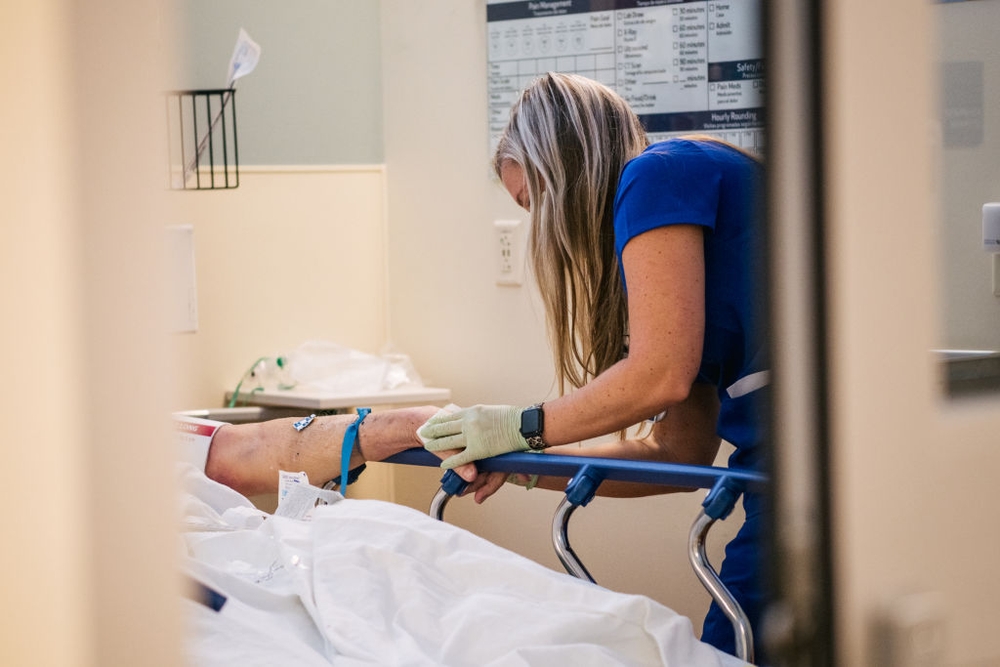
The Alarming State of Rural Healthcare in Missouri
Missouri faces a devastating rural healthcare crisis that demands urgent attention from policymakers and citizens alike. According to the Center for Healthcare Quality and Payment Reform, 50% of Missouri’s 58 remaining rural hospitals are at risk of closure, with another 21% considered at immediate risk. These institutions represent far more than just medical facilities—they serve as emergency rooms, labor and delivery units, and the only accessible care for stroke patients within an hour’s drive for many communities. The legislature correctly recognizes this as a crisis, but their proposed solution raises serious constitutional and ethical concerns that could exacerbate rather than alleviate the problem.
The Proposed Legislative Response
The Missouri House Special Committee on Rural Issues recently advanced legislation that would authorize MU Health Care to acquire hospitals across 25 rural counties surrounding Columbia. What makes this legislation particularly concerning is its grant of sweeping immunity from federal and state antitrust laws for MU Health Care and collaborating entities operating in this 25-county region. The bill explicitly states that Missouri “affirmatively expresses a policy” allowing these activities “notwithstanding that such activities may have the effect of displacing competition.” This immunity extends not only to the university system but also to “any public or private entities and individuals” working with it.
Most alarmingly, this two-page legislation contains no rate transparency requirements, no commitments to maintain essential services such as emergency care or obstetrics, no reporting obligations, and no agency designated to supervise pricing or market conduct after acquisitions occur. While the bill preserves liability for violations such as price-fixing and bid-rigging, it creates no affirmative oversight structure governing consolidation within the region. Existing certificate-of-need law still applies, but no new supervisory framework governs pricing, service obligations, or post-acquisition market conduct.
Comparative Analysis with Other States
Other states that grant antitrust immunity for hospital consolidation typically pair it with robust regulatory oversight through certificate-of-public-advantage frameworks. Tennessee’s Ballad Health merger includes pricing limits, reporting requirements, a compliance office, and an independent monitor—though Tennessee’s experience also demonstrates that oversight requires genuine enforcement. Ballad has missed roughly three-quarters of its quality benchmarks for years, and the state has repeatedly waived charity care obligations and allowed quality failures to persist rather than acting on them.
Virginia requires annual reporting and a yearly determination that a merger’s benefits continue to outweigh the harms of reduced competition. Indiana allows a cooperative agreement only if the state’s Department of Health finds clear evidence that consolidation will improve outcomes, access, and quality enough to outweigh the loss of competition. West Virginia places similar agreements under review by its Health Care Authority. Missouri’s bill conspicuously lacks this kind of post-acquisition supervision built into the statute.
The Dangers of Unchecked Consolidation
Research on hospital consolidation shows a consistent and troubling pattern: when competition shrinks, prices tend to rise dramatically. The U.S. Department of Health and Human Services reported in 2025 that hospital consolidation increases commercial prices by 6% to 65% in concentrated markets. Evidence on quality outcomes is largely negative, with more than half of studies finding worse outcomes or no change, and only about one in five showing modest gains.
The Federal Trade Commission raised similar concerns in a 2023 letter opposing North Carolina legislation that would have granted a public university health system broad antitrust immunity—a warning that reflects longstanding bipartisan consensus on hospital consolidation. The agency warned that such legislation can authorize acquisitions that reduce competition and lead to higher costs, lower quality, and reduced access—precisely the concerns raised by Missouri’s proposed legislation.
A Constitutional and Ethical Imperative for Better Solutions
As someone deeply committed to democratic principles, constitutional governance, and human dignity, I find this legislative approach profoundly troubling. While the crisis is real and requires urgent action, replacing competition with unchecked consolidation without adequate safeguards violates fundamental principles of good governance and patient protection. The legislature’s approach essentially creates a healthcare monopoly in these 25 counties without establishing the necessary oversight to prevent abuse.
The bill’s sponsors are responding to a genuine problem—even some lawmakers like State Rep. Kent Haden have reservations, calling the bill a “double-edged sword” and noting he represents a healthcare desert himself. However, good intentions cannot excuse poor policy design. When a legislature replaces competition by statute, the price discipline that competition provides disappears, potentially leaving patients facing higher prices, fewer choices, and reduced service options when a single system dominates a region.
A Path Forward with Proper Safeguards
Missouri lawmakers could and should designate the Missouri Department of Health and Senior Services to approve acquisitions within the 25-county zone, attach conditions on pricing and service obligations, require biennial public reporting, and retain authority to modify or revoke immunity if those conditions are not met. Unlike Tennessee’s rubric-based scoring system, which allowed Ballad to miss benchmarks for years without consequence, Missouri could build in automatic revocation triggers tied to specific, measurable conditions—approaches already used in Tennessee, Virginia, Indiana, and West Virginia.
Rural hospitals desperately need stability, and patients need protection from unchecked consolidation. Missouri can provide both—but only if lawmakers add the safeguards other states already require. This isn’t just about healthcare policy; it’s about fundamental principles of good governance, constitutional protection of citizens’ welfare, and the ethical obligation to ensure that vulnerable populations don’t bear the burden of poorly designed legislation.
The current approach represents a dangerous abandonment of oversight responsibility that could have devastating consequences for rural Missourians. We must demand better from our elected officials—policies that address the crisis while protecting patients’ rights, ensuring affordability, and maintaining quality care. The health of our rural communities and the principles of good governance demand nothing less.
